 
That was done, I stopped all the bleeding with a cautery, packed the incision, and then on to part 2 of the surgery, which is taking out the lymph nodes under the arm to see if there's been any spread of tumor to the underarm lymph nodes.įor that, there was the second incision placed in the underarm. I then resumed the normal part of the procedure, which was I did some cosmetic work lifting the breast tissue off the muscle, so I could mobilize it in a local advancement flap to get a better closure cosmetically. There was one spot in the deep margin where there was some signal, uh, fluorescent signal, that had me take a second margin in that area and after that, that area looked clean. And then after that, the machine, uh, algorithms calculated what that patient's threshold was for normal versus tumor, and I then went back and systematically looked at the cavity, uh, with the machine applying the threshold. We got the patient's baseline measurements, just looking all around first at 6 surfaces of the cavity. It also is more precise for orienting where any part - positive margins might be, as compared to just using marking stitches or paint on the original specimen.Īfter we did that, we did the protocol part of the study, which is where I introduce the Lumicell probe into the cavity. Uh, we do that because randomized studies have shown that that cuts the re-excision rate in half, and that makes up for any trauma to the specimen that can make a margin look positive when it actually isn't. That's taking a thin shave of tissue from the cavity that's the left after that first lumpectomy has been removed. I then went back and did the standard of care here at MGH, which is taking comprehensive shaved margins of the entire cavity. And that picture showed us that the lesion was pretty well centered in the lumpectomy specimen I took out, and it looked like there was grossly clear tissue all the way around. We had put metallic markers on, so we would be able to orient the specimen on the X-ray image relative to where the tumor was in the patient. 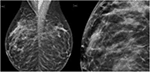
Um, and then once the main specimen was out, we actually imaged it in the operating room. We did that as the first step in the surgery, took the tumor out after we made the incision, exposed it circumferentially to make that easier. Uh, her tumor was palpable, so I was able to use touch to put my hand on the tumor and cut about 1 cm or 1.5 cm all the way around. Other than that, it was quite a standard lumpectomy, where the idea was to take out her tumor, uh, with a margin of normal-appearing tissue around it. The things you saw us do that were using this imaging device, uh, covering things with a towel, turning the lights on and off, that was all part of the protocol. The key things of this is she was injected with a dye before she got to the operating room, that was going to - the lume 015 dye, that becomes activated to a fluorescent form in areas where there's tumor. So, preop, this is a woman with a palpable breast cancer, and she agreed to be in our study, where we're trying to find ways to detect residual tumor during the first operation and not leave any tumor behind, and not have to do second surgeries. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
